The study of human anatomy is a journey into the most complex biological machine in existence. For centuries, the primary challenge for students of medicine, art, and anthropology has been the ability to visualize the internal structures that provide the human body with its shape, protection, and mobility. In the modern educational landscape, the physical representation of these structures has become a cornerstone of effective learning. While digital textbooks and virtual reality offer impressive visualizations, the tactile experience and spatial accuracy of a physical model remain indispensable. Among the various tools available to the modern educator, the detailed study of the cranium and the complete framework of the body provide the most profound insights into human physiology.
The Cranium as a Masterpiece of Biological Engineering
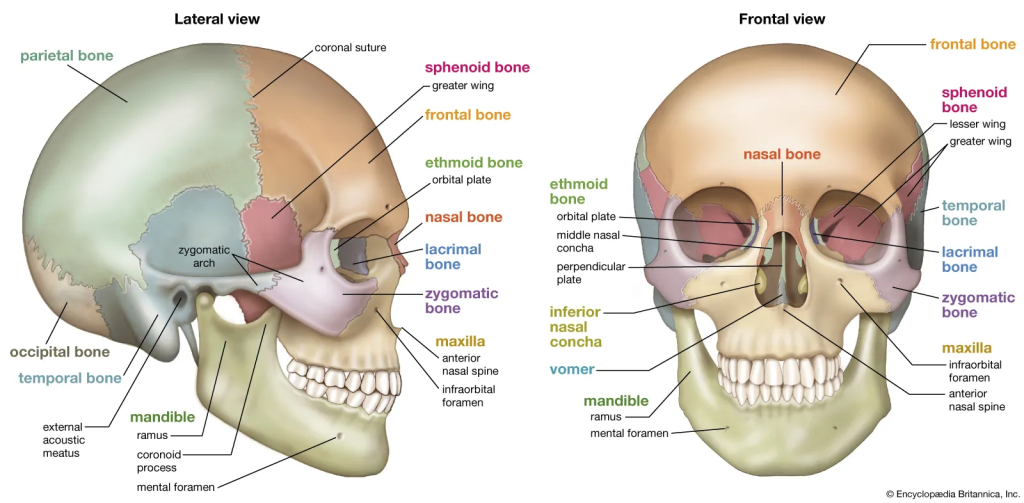
The human skull is far more than a simple protective casing for the brain. It is a highly complex assembly of twenty-two individual bones, joined by intricate sutures that allow for minor adjustments during growth while maintaining incredible structural integrity. Understanding the relationship between these bones is a fundamental requirement for anyone entering the fields of neurology, dentistry, or craniofacial surgery. However, the internal geography of the skull—including the various foramina that allow for the passage of cranial nerves and blood vessels—is notoriously difficult to master through two-dimensional illustrations alone.
This is where the precision of a high-quality anatomy skull model becomes vital. A physical model allows a student to trace the path of the trigeminal nerve or visualize the depth of the orbital sockets in three dimensions. Modern manufacturing techniques have reached a point where these models can replicate the exact weight, texture, and density of human bone. Some advanced versions feature removable parts, such as a detachable calvarium or a spring-loaded mandible, allowing for an internal examination of the sphenoid and ethmoid bones. By physically manipulating these parts, learners transition from memorizing names to understanding the mechanical and spatial relationships that define human life.
The Framework of Movement and Stability
While the skull protects our most vital organ, the rest of the skeletal system provides the structural foundation that makes movement possible. The human skeleton is a dynamic system that serves as a reservoir for minerals, a factory for blood cells, and a sophisticated lever system for our muscles. For a physical therapist, an orthopedic surgeon, or a sports medicine specialist, a deep understanding of how these 206 bones interact is mandatory. The subtle curves of the vertebral column, the complex articulation of the pelvic girdle, and the delicate arrangement of the carpal bones in the wrist cannot be fully appreciated without a physical reference.
The use of a full-scale anatomy skeleton model provides the necessary context for systemic study. Having a life-size representation in the laboratory allows students to appreciate the scale of the human body and the proportions between different limbs. These models are typically articulated to demonstrate natural ranges of motion, making them excellent tools for explaining joint mechanics and the origins of common injuries. For instance, demonstrating the difference between a hinge joint and a ball-and-socket joint becomes an intuitive process when a student can physically move the humerus within the glenoid cavity. This tactile feedback bridges the gap between the abstract descriptions found in a textbook and the physical reality of a living patient.
Cognitive Benefits of Physical Interaction in Medical Pedagogy
Educational psychology has long noted that the human brain is wired for spatial and tactile learning. The act of touching a physical object and viewing it from multiple angles creates a more robust “mental map” than viewing a flat image on a screen. When a student handles a model, they are engaging their kinesthetic memory. This is particularly important in medical education, where the ability to palpate landmarks and recognize shapes by touch is a critical diagnostic skill.
Furthermore, physical models encourage collaborative learning. In a classroom setting, a group of students can gather around a skeletal model to discuss the insertion points of muscles or the potential pathways of a traumatic injury. This shared physical space fosters communication and peer-to-peer teaching, which are essential components of modern medical training. Unlike a digital screen, which is often a solitary experience, a physical model is a communal resource that brings the subject matter to life in a way that encourages active inquiry.
Bridging the Gap in Patient Communication
The utility of anatomical modeling extends far beyond the university lecture hall. In the clinical environment, these tools serve as powerful bridges for communication between healthcare providers and their patients. Medical conditions are often abstract and frightening concepts for those without specialized training. When a physician uses a physical model to explain a diagnosis—such as a disc herniation in the spine or a fracture in the hand—the patient’s level of understanding increases exponentially.
By using a physical model, a clinician can demonstrate exactly where a procedure will take place and what the expected outcomes will be. This visual and tactile aid reduces patient anxiety and fosters a sense of informed consent. When a patient can see and touch a representation of their own anatomy, they feel more empowered in their healthcare journey. This clarity leads to better treatment compliance and a stronger relationship between the patient and the medical team, ultimately improving the quality of care.
Durability and Technical Precision in Manufacturing
One of the most significant advancements in the field of anatomical modeling is the improvement in material science. Early models were often made of fragile wax or heavy plaster, which limited their use in high-traffic educational settings. Today, medical-grade plastics and resins are used to create models that are almost indestructible while maintaining a level of detail that rivals real bone. These materials allow for the replication of subtle surface features like grooves for blood vessels and rough attachment points for ligaments.
This technical precision is what differentiates a toy from a medical-grade educational instrument. A high-quality model is cast from real human specimens, ensuring that the proportions and landmarks are anatomically correct. This accuracy is paramount; a model that misrepresents the size of a foramen or the curvature of a rib can lead to fundamental misunderstandings that could have serious implications in a clinical setting. Therefore, investing in professionally crafted models is a commitment to the accuracy and integrity of the educational process.
The Enduring Value of Tangible Education
As we move further into a world dominated by digital interfaces, the value of the tangible becomes even more apparent. The human body is a physical entity, and its study requires a physical medium. Anatomical models represent a legacy of scientific inquiry that dates back to the earliest medical pioneers, but they have been refined by the technology of the twenty-first century.
Whether it is for the meticulous study of the cranial nerves or the broader understanding of human biomechanics, these models provide a constant, reliable reference point. They do not require a battery, an internet connection, or a software update. They are always ready to serve as silent mentors to the next generation of healers and scientists. By grounding the study of anatomy in the physical world, we ensure that our understanding of ourselves remains accurate, profound, and deeply human. The interplay between the hard structures of the bone and the soft tissues they support is the story of our survival, and there is no better way to tell that story than through the high-fidelity representation of the human skeleton.